Warning: Illegal string offset 'source_type' in /home/mychutej/public_html/blog/wp-content/plugins/egany-facebook-to-wp/egany_facebook_to_wordpress.php on line 1099
Large populations across borders affected, over 6800 lives lost, hundreds of new infections daily. Over a billion dollars in estimated expenditure on direct health costs, human resources and logistics from numerous governments, international organizations and not for profit foundations. Millions more have been spent on research on vaccines and drugs.
Little is known on the exact social costs of this illness-a toll too grave to imagine.
History speaks to us of several diseases that have ravaged mankind. From the Bubonic plague of the Middle Ages, to Smallpox, and most recent in human memory – Malaria and HIV, two diseases whose battles we still fight.
Our strategy for tackling pandemics was simple – find the “who”, “why” and “how” of the disease, and science would wrestle it till successful prevention is achieved, or a cure is found.
Ebola shares some similarities with these battles – a seemingly unhalted spread across population groups, a short course of progression and devastating effects. With humanity’s experience at tackling diseases, why would Ebola prove so deadly?
The weakness of existing health systems in the region with the highest mortality rates is the strongest factor. This weakness in health systems is directly attributable to a history of conflict and failed administrations common to the three affected nations.
A recovery from state failure precipitated a dependence on foreign loans with attendant stringent directives -a recent study published stated that these were targeted majorly at boosting the foreign reserves, with less priority given to the much needed development in key sectors particularly healthcare and education.
The long course of underfunding, juxtaposed policies and continued decentralization and privatization have taken a large toll on the human resources available for health. The WHO Country Health Profiles record Guinea with no doctors per 10,000 population, Liberia as 0.1 per 10,000 and Sierra Leone as 0.2 per 10,000 population. This compares poorly with a regional average of 2.6 per 10,000.
In addition, allegations of misappropriation of funds and a reduced investment in public infrastructure have created problems of inadequate transportation and a reduced access to non-industrialized areas. In Sierra Leone for instance, sixty percent of the population resides in rural areas. The same goes for Liberia and Guinea with figures of fifty-one percent and sixty-four percent respectively.
Furthermore, rising Healthcare costs have resulted in an increase in the patronage of unorthodox health practitioners, a practice that continues to this day. International news feeds over the course of the outbreak ran abuzz with stories of traditional practitioners promising cures and discouraging the population from accessing hospitals.
Supervening cultural and religious norms have also contributed in various ways to this epidemic. Ebola is spread through close physical contact with infected people. For many in the affected countries this is a problem as practices around religion and death involve close physical contact. Hugging is a normal part of religious worship in Liberia and Sierra Leone, and across the region the ritual preparation of bodies for burial involves washing, touching and kissing. Those with the highest status in society are often charged with washing and preparing the body. For a woman this can include braiding the hair, and for a man shaving the head.
This deadly virus has been able to home in on illiteracy, poor health practices and a distrust for governmental intentions, all on a background of administrations undergoing much needed reforms.
The course of the present epidemic is a wake-up call to countries with underdeveloped health systems. The African continent has several peculiarities, manifested in various ways in her nations. These must be fully resolved to enable better handling of emergencies -health and otherwise. The attendant fears of any epidemic in Africa will not be laid to rest until these gaps are bridged.
Ria Evbuoma.
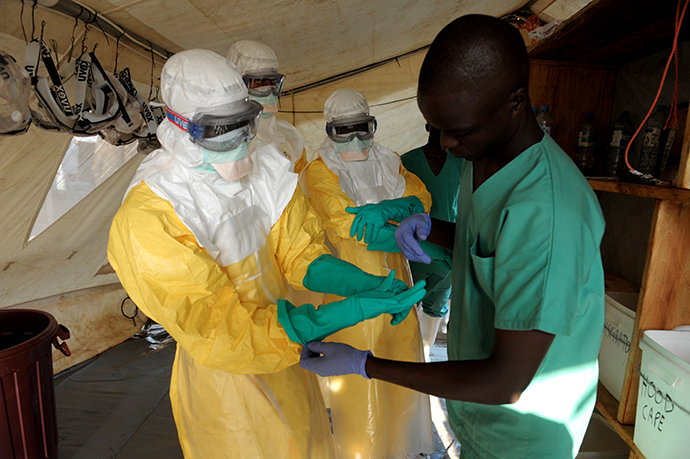
Photo Credit: AFP PHOTO / SEYLLOU












April 11, 2015 at 9:21 pm
Hi, my name is Catherine and I am the sales manager at StarSEO Marketing. I was just looking at your Why is Ebola so deadly? | EbolaAlert Blog site and see that your site has the potential to become very popular. I just want to tell you, In case you don’t already know… There is a website service which already has more than 16 million users, and most of the users are looking for niches like yours. By getting your website on this service you have a chance to get your site more popular than you can imagine. It is free to sign up and you can read more about it here: http://cabkit.in/9mt5 – Now, let me ask you… Do you need your site to be successful to maintain your way of life? Do you need targeted visitors who are interested in the services and products you offer? Are looking for exposure, to increase sales, and to quickly develop awareness for your website? If your answer is YES, you can achieve these things only if you get your website on the network I am talking about. This traffic network advertises you to thousands, while also giving you a chance to test the service before paying anything. All the popular sites are using this network to boost their traffic and ad revenue! Why aren’t you? And what is better than traffic? It’s recurring traffic! That’s how running a successful website works… Here’s to your success! Read more here: http://cabkit.in/9mt5
April 24, 2015 at 8:59 pm
I see many websites outrank your website in google’s
search results. You should build more contextual backlinks.
These type of backlinks are the best after all these google algorithm updates.
Writing content is hard work, but i know what tool will save you a lot of time.
This tool can also make you money, just search in google for:
Haough’s Essential Tool
May 4, 2015 at 5:25 am
act now apologize later
May 13, 2015 at 12:53 pm
Hi my name is Olivie and I just wanted to drop you a quick note here instead of calling you. I came to your Why is Ebola so deadly? | EbolaAlert Blog page and noticed you could have a lot more hits. I have found that the key to running a popular website is making sure the visitors you are getting are interested in your subject matter. There is a company that you can get targeted traffic from and they let you try the service for free for 7 days. I managed to get over 300 targeted visitors to day to my site. Check it out here: http://9n3.us/7uza
May 13, 2015 at 10:56 pm
Hi, my name is Brigitte and I am the sales manager at SwingSEO Solutions. I was just looking at your Why is Ebola so deadly? | EbolaAlert Blog website and see that your site has the potential to become very popular. I just want to tell you, In case you don’t already know… There is a website service which already has more than 16 million users, and most of the users are interested in topics like yours. By getting your site on this service you have a chance to get your site more visitors than you can imagine. It is free to sign up and you can find out more about it here: http://claimyourexcellence.info/24o – Now, let me ask you… Do you need your site to be successful to maintain your business? Do you need targeted visitors who are interested in the services and products you offer? Are looking for exposure, to increase sales, and to quickly develop awareness for your site? If your answer is YES, you can achieve these things only if you get your website on the service I am describing. This traffic service advertises you to thousands, while also giving you a chance to test the network before paying anything. All the popular blogs are using this service to boost their traffic and ad revenue! Why aren’t you? And what is better than traffic? It’s recurring traffic! That’s how running a successful website works… Here’s to your success! Find out more here: http://qa.juststicky.com/yourls/278u – or to unsubscribe please go here: http://todochiapas.mx/C/36p
May 18, 2015 at 12:24 pm
Hello siblings loves your terrific article and pls stick at it
May 19, 2015 at 4:03 am
Thank you for your useful informative article. I feel I’ve come away a little smarter and more open-minded by reading your article. I am saving your article to my favorites to show to my family.
June 23, 2015 at 12:33 am
Heya i’m for the first time here. I found this board and I
find It really useful & it helped me out much.
I hope to give something back and aid others like you aided me.
July 19, 2015 at 6:02 pm
Highly energetic article, I liked that bit. Will there be a part 2?
July 25, 2015 at 5:43 pm
Good answer back in return of this matter with real arguments and describing everything on the topic of that.
July 27, 2015 at 10:34 am
I was just looking at your Why is Ebola so deadly? | EbolaAlert Blog website and see that your website has the potential to become very popular. I just want to tell you, In case you don’t already know… There is a website service which already has more than 16 million users, and most of the users are looking for websites like yours. By getting your website on this network you have a chance to get your site more popular than you can imagine. It is free to sign up and you can read more about it here: http://bbqr.me/4fj5 – Now, let me ask you… Do you need your website to be successful to maintain your way of life? Do you need targeted traffic who are interested in the services and products you offer? Are looking for exposure, to increase sales, and to quickly develop awareness for your site? If your answer is YES, you can achieve these things only if you get your website on the network I am describing. This traffic service advertises you to thousands, while also giving you a chance to test the service before paying anything at all. All the popular blogs are using this network to boost their traffic and ad revenue! Why aren’t you? And what is better than traffic? It’s recurring traffic! That’s how running a successful website works… Here’s to your success! Find out more here: http://claimyourexcellence.info/12ny
July 27, 2015 at 4:57 pm
Howdy! Do you know if they make any plugins to safeguard against hackers?
I’m kinda paranoid about losing everything I’ve worked hard
on. Any recommendations?
July 28, 2015 at 7:16 pm
Howdy! I could have sworn I’ve been to this blog before but after checking through some of the post I realized it’s new to me.
Anyways, I’m definitely glad I found it and I’ll be bookmarking and checking back often!
July 29, 2015 at 3:44 pm
Wow, marvelous blog layout! How long have you been blogging
for? you make blogging look easy. The overall look of your site
is magnificent, as well as the content!
July 30, 2015 at 2:59 pm
I absolutely love your blog.. Great colors & theme.
Did you create this site yourself? Please reply back as I’m attempting to create my very own website
and want to find out where you got this from or what
the theme is named. Kudos!